Category: Females • Page 2
-
There is a significant burden of chronic pain in trans-identified individuals, with an increased risk among those receiving cross-sex hormones
A 2024 large US clinical database study1 of 98,352 trans-identified individuals (56,470 females and 41,882 males) found significantly higher rates of chronic pain compared to the general population. Of particular concern, those receiving cross-sex hormones showed even higher risks – females on testosterone had a 20% increased hazard of chronic pain diagnosis compared to those not taking testosterone, while males on estrogen showed a 19.4% increased risk.
- Tabernacki, T., Gilbert, D., Rhodes, S., Scarberry, K., Pope, R., McNamara, M., … & Mishra, K. (2024). The burden of chronic pain in transgender and gender diverse populations: Evidence from a large US clinical database. European Journal of Pain. [Link] ↩︎
-
Genital masculinizing surgeries rose by 424% and feminizing surgeries by 343% in Germany between 2006 and 2022
A 2024 German national study1 analyzing hospital records found that genital “gender-affirming” surgeries increased nearly 5-fold between 2006 and 2022. Masculinizing surgeries showed the most dramatic increase at 424%, with their highest annual rise occurring between 2018-2019, while feminizing surgeries increased by 343%, with their steepest rise between 2015-2016. The study found a dramatic shift toward younger patients, with over 70% of masculinizing and about half of feminizing surgeries performed on people aged 20-34 in 2022, compared to about a quarter for both types in 2006. These procedures became increasingly concentrated in specialized centers, with half of hospitals performing over 50 masculinizing surgeries annually by 2022, up from 15% in 2006.
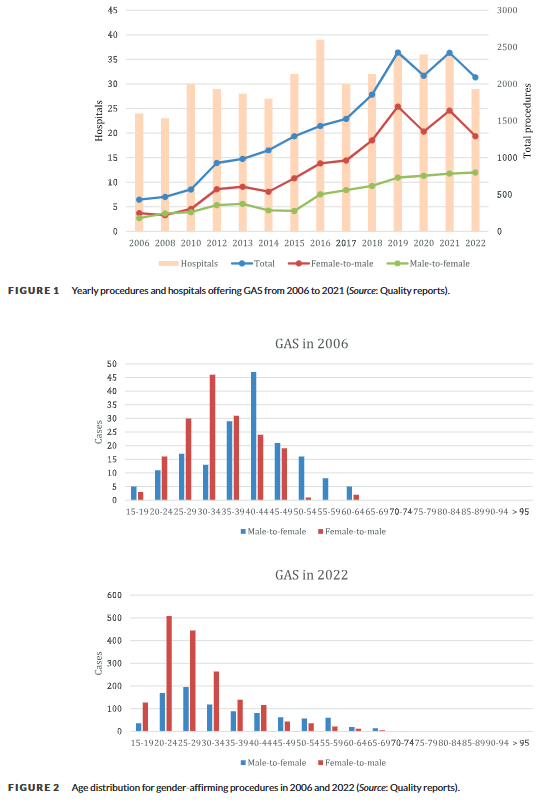
- Aksoy, C., Wellenbrock, S., Reimold, P., Karschuck, P., Ozturk, M., Hirsch, T., … & Flegar, L. (2024). Genital gender‐affirming surgery trends in Germany: Total population data with 19,600 cases from 2006 to 2022. Andrology. [Link] ↩︎
-
Long term use of male sex hormones in females is deleterious to their health
The state-sponsored doping program of the German Democratic Republic (GDR) systematically administered androgens and other drugs to several thousand athletes, including minors, from 1966 onwards, leading to harmful side effects such as virilization in adolescent girls and female athletes, and other damaging effects that required medical and surgical interventions1.
Initiated in 1966, the German Democratic Republic (GDR) embarked on an extensive state-sponsored doping program. This program involved the systematic delivery of androgens and other substances to thousands of athletes, some of whom were minors. Women and adolescent girls were at the core of this program as the introduction of androgens was discovered to dramatically enhance their athletic performance. The ensuing side effects, including virilization in females, were deleterious and often so severe that they required medical and surgical responses. The program’s existence was only unveiled with the fall of the GDR in 1990, through the recovery of preserved classified documents.
- Franke, W. W., & Berendonk, B. (1997). Hormonal doping and androgenization of athletes: a secret program of the German Democratic Republic government. Clinical chemistry, 43(7), 1262-1279. [Link] ↩︎
-
Long term testosterone use potentially compromises fertility and negatively affects ovarian follicle health
One study in 2023 found that long-term testosterone exposure, as seen in transgender men undergoing gender-affirming therapy, could potentially compromise fertility by negatively affecting ovarian follicle growth, health, and DNA integrity.
In 2023, a study by Bailie et al1. explored the effects of long-term testosterone exposure on ovarian follicles in transgender men receiving gender-affirming endocrine therapy. The research indicated that testosterone was linked with decreased follicle growth activation, poor follicle health, and increased DNA damage, suggesting possible impacts on fertility. Further, these negative effects were intensified following six days of in vitro culture. These findings may have crucial implications for reproductive health and fertility considerations among transgender men receiving testosterone as part of their gender-affirming therapy.
- Bailie, E., Maidarti, M., Hawthorn, R., Jack, S., Watson, N., Telfer, E. E., & Anderson, R. A. (2023). The ovaries of transgender men indicate effects of high dose testosterone on the primordial and early growing follicle pool. Reproduction and Fertility, 4(2). [Link] ↩︎
-
60% of males and 70% of females attending the world’s largest gender clinic (GIDS) are same-sex attracted
In the 2015 statistics from GIDS, approximately 60% of the youth seen there who were biological males and 70% who were biological females reported attraction to the same sex or to both sexes1.
The 2015 Gender Identity Development Service (GIDS) statistics revealed a notably high rate of same-sex attraction among the youth seen at their clinic. Over half of the biological females reported same-sex attraction, about 20% were attracted to both sexes, and a quarter to the opposite sex, with the remaining identifying as asexual. Among biological males, approximately 30% reported same-sex attraction, another 30% to both sexes, 30% to the opposite sex, with the last 10% identifying as asexual or reporting no sexual attraction.
Download as PDF -
It is not true that 1.7% of the population is ‘born between the sexes’. The proportion of people with DSDs (‘intersex’ conditions) is 0.018%
Conditions in which chromosomal sex is inconsistent with phenotypic sex, or in which the phenotype is not classifiable as either male or female, occur in 0.018% of the population1.
The claim that 1.7% of the population is ‘intersex’2 includes conditions which most clinicians do not recognize as intersex, and is often wrongly used to back up the ideological assertion that ‘sex is a spectrum’, or that biological sex is not dimorphic.
The philosopher Kathleen Stock points out that she would be considered as “intersex” under Fausto-Sterling’s “preposterously over-demanding conditions on sex category membership”, as she lost an ovary in early adulthood3, which would count as “intersex” according to Fausto-Sterling.
- Sax, L. (2002). How common is intersex? a response to Anne Fausto-Sterling. J Sex Res. 39 (3): 174-8. [Link] ↩︎
- Fausto-Sterling, A. (2000). Sexing the Body: Gender Politics and the Construction of Sexuality. New York: Basic Books. [Link] ↩︎
- Stock, K. (2021). Material Girls. Little, Brown Book Group: p.56 [Link] ↩︎
-
There are 2 sexes: male and female. Biological sex is not a spectrum
According to an Endocrine Society Scientific Statement1,
Sex is dichotomous, with sex determination in the fertilized zygote stemming from unequal expression of sex chromosomal genes.
Sex differences in baseline physiology and associated mechanisms form the foundation for understanding sex differences in diseases pathology, treatments, and outcomes.
The erroneous claim that biological sex is a spectrum, or non-dichotomous, is often used to justify the ideological assertion that all humans are ‘assigned sex at birth’. In fact, biological sex is encoded in every cell of the body2.
- Bhargava, A., Arnold, A.P., Bangasser, D.A., Denton, K.M., Gupta, A., Hilliard Krause, L.M., Mayer, E.A., McCarthy, M., Miller, W.L., Raznahan, A. & Verma, R. (2021). Considering Sex as a Biological Variable in Basic and Clinical Studies: An Endocrine Society Scientific Statement. Endocrine Reviews 42 (3): 219-258. [Link] ↩︎
- Shah, K. McCormack, C. & Bradbury, N. (2014). Do you know the sex of your cells?’ American Journal of Physiology – Cell Physiology, C3-C18, 306, 1. [Link] ↩︎
-
In one study of detransitioners, males were three times more likely than females to have transitioned for erotic reasons
In a study1 of 100 detransitioners, 38.7% of males identified with the comment “I had erotic reasons for wanting to transition”.
The figure for females was a third of this, at 13%.
- Littman, L. (2021). Individuals Treated for Gender Dysphoria with Medical and/or Surgical Transition Who Subsequently Detransitioned: A Survey of 100 Detransitioners. Arch Sex Behav. [Link] ↩︎
-
In one study, female detransitioners were three times more likely to be lesbians than to be straight
A study1 of 100 detransitioners, the majority of whom were female, showed that 26.1% of the females were homosexual before they transitioned.
Only 8.7% considered themselves heterosexual.
- Littman, L. (2021). Individuals Treated for Gender Dysphoria with Medical and/or Surgical Transition Who Subsequently Detransitioned: A Survey of 100 Detransitioners. Arch Sex Behav. [Link] ↩︎
-
Transmen are four or five times more likely than females in general to suffer a heart attack
A 2019 study1 found that post-operative female-to-male transgender people were 4.9 times as likely to suffer a myocardial infarction (heart attack) than women in general.
Another study2 also found a somewhat smaller yet still large discrepancy, concluding that transmen were 3.69 more likely to suffer a heart attack than women in general.
- Alzahrani, T. Nguyen, T., Ryan, A., Dwairy, A. McCaffrey, J., Yunus, R., Forgione, J., Krepp, J., Nagy, C., Mazhari, R. & Reiner, J. (2019). Cardiovascular Disease Risk Factors and Myocardial Infarction in the Transgender Population. Circulation: Cardiovascular Quality and Outcomes 12 (4). [Link] ↩︎
- Nota, N.M., Wiepjes, C.M., de Blok, C.J.M., Gooren, L.J.G., Kreukels, B.P.D. & den Heijer, M. (2019). Occurrence of Acute Cardiovascular Events in Transgender Individuals Receiving Hormone Therapy: Results From a Large Cohort Study. Circulation 139: 1461-1462. [Link] ↩︎
-
There is evidence that up to a quarter of transgender genital surgeries result in incontinence
A systematic literature review1 found that 21% of male-to-female patients and 25% of female-to-male patients suffered from incontinence as a result of transgender genital surgery.
One recent study2 estimates the number of post-operative transsexuals suffering stress incontinence to be 23%. This study was not a literature review, and almost all of the participants were male-to-female.
- Nassiri, N., Maas, M., Basin, M., Cacciamani, G.E. & Doumanian, L.R. (2020). Urethral complications after gender reassignment surgery: a systematic review. Int J Impot Res. [Link] ↩︎
- Kuhn, A., Santi, A. & Birkhäuser, M. (2011). Vaginal prolapse, pelvic floor function, and related symptoms 16 years after sex reassignment surgery in transsexuals. Fertil Steril. 95: 2379-82. [Link] ↩︎
-
Genital surgeries tend to reduce the capacity for orgasm in males, and may do so in females
One study showed that around 30% of male-to-female genital surgeries result in the inability to orgasm1.
Figures on female-to-male transitioners are less clear. However, a clinical follow-up study2 of 38 transmen – 29 of whom had received phalloplasty, and 9 metoidioplasty – found that reported loss of orgasmic capacity was more marginally common than reported gain of orgasmic capacity.
The negative intrapsychic and interpersonal consequences of anorgasmia (the inability to climax) is well-documented, and applies equally to transgender individuals3.
- Manrique, O., Adabi, K., Martinez-Jorge, J., Ciudad, P., Nicoli, F. and Kiranantawat, K. (2018). Complications and Patient-Reported Outcomes in Male-to-Female Vaginoplasty—Where We Are Today. Annals of Plastic Surgery 80 (6): 684-691. [Link] ↩︎
- van de Grift, T., Pigot, G., Kreukels, B., Bouman, M., & Mullender, M. (2019). Transmen’s Experienced Sexuality and Genital Gender-Affirming Surgery: Findings From a Clinical Follow-Up Study. Journal Of Sex & Marital Therapy 45 (3): 201-205. [Link] ↩︎
- Levine, S. (2018). Informed Consent for Transgendered Patients. Journal Of Sex & Marital Therapy, 45(3), 218-229. [Link] ↩︎
-
In one study, 11% of transmen who took testosterone developed a condition called erythrocytosis, which impacts red blood cells and slows the blood flow
A study1 of 776 transmen who took testosterone demonstrated that 11% of them developed erythrocytosis, a condition which slows the blood flow, and can lead to headaches, confusion, high blood pressure, nosebleeds, blurred vision, itching and fatigue.
- Madsen, M.C., van Dijk, D. Wiepjes, C.M., Conemans, E.B., Thijs, A. & den Heijer, M. (2021). Erythrocytosis in a Large Cohort of Trans Men Using Testosterone: A Long-Term Follow-Up Study on Prevalence, Determinants, and Exposure Years. The Journal of Clinical Endocrinology & Metabolism 106 (6): 1710–1717. [Link] ↩︎
-
Long-term testosterone use in natal females can cause vaginal atrophy, which makes sex painful
A study1 of 16 female-to-male transgender individuals concluded that long-term testosterone administration leads to vaginal atrophy (Baldassarre et al., 2013). The study noted that:
Vaginal samples from FtM showed a loss of normal architecture of the epithelium, intermediate and superficial layers were completely lost, and glycogen content was depleted.
Vaginal atrophy, characterized by thinning of vaginal walls and poor lubrication of vaginal tissues, leads to tearing, micro abrasions, bleeding, and painful intercourse.
- Baldassarre, M., Giannone, F., Foschini, M., Battaglia, C., Busacchi, P., Venturoli, S., & Meriggiola, M. (2013). Effects of long-term high dose testosterone administration on vaginal epithelium structure and estrogen receptor-α and -β expression of young women. International Journal Of Impotence Research, 25 (5): 172-177. [Link] ↩︎
-
A study which looked at 27 different negative health effects of binding found that some do not show for years
A survey1 of 1800 females who used breast binders reported a number of negative health effects which develop over time. Some of these effects are felt immediately. However, in other cases, it can take years for the negative health effects to be fully seen:

- Peitzmeier, S.M., Silberholz, J., Gardner, I.H., Weinand, J. & Acevedo, K. (2021). Time to First Onset of Chest Binding-Related Symptoms in Transgender Youth. Pediatrics 147 (3). [Link] ↩︎
-
There is evidence that chest binding has a statistically significant impact on lung function
A study1 found that:
Transgender individuals using chest binders have abnormal lung function. The acute effect of wearing the binder appears to be an overall volume reduction with little other change.
- Cumming, R., Sylvester, K. & Fuld, J.P. (2016). Understanding the effects on lung function of chest binder use in the transgender population. Thorax 71. [Link] ↩︎
-
There is an array of negative health effects associated with chest binding
There is a range of negative effects which chest binding can cause1.
A survey2 of transmen who engaged in breast binding found that 68% were concerned about the health effects. The most common symptoms associated with binding were back pain (65%), shortness of breath (48.6%), bad posture (32%), chest pain (30%), and light-headedness (30%).
- Peitzmeier, S., Gardner, I., Weinand, J., Corbet A. & Acevedo, K. (2017). Health impact of chest binding among transgender adults: a community-engaged, cross-sectional study. Culture, Health & Sexuality 19 (1): 64-75. [Link] ↩︎
- Poteat, T., Malik, M., & Cooney, E. (2018). Understanding the health effects of binding and tucking for gender affirmation. Journal of Clinical and Translational Science 2 (Suppl 1), 76. [Link] ↩︎
-
Medical transition puts both males and females at risk of infertility
A wide-ranging study1 found that gender-related drug regimens place patients at risk of infertility:
Suppression of puberty with gonadotropin-releasing hormone agonist analogs (GnRHa) in the pediatric transgender patient can pause the maturation of germ cells, and thus, affect fertility potential. Testosterone therapy in transgender men can suppress ovulation and alter ovarian histology, while estrogen therapy in transgender women can lead to impaired spermatogenesis and testicular atrophy. The effect of hormone therapy on fertility is potentially reversible, but the extent is unclear.
On surgeries, the study noted that cross-sex surgery that includes hysterectomy and oophorectomy in transmen or orchiectomy in transwomen results in permanent sterility.
- Cheng, P.J., Pastuszak, A.W., Myers, J.B., Goodwin, I.A. & Hotaling, J.M. (2019). Fertility concerns of the transgender patient. Transl Androl Urol. 8 (3): 209-218. [Link] ↩︎
-
Female-to-male genital reconstruction surgery has a high negative outcome rate, including urethral compromise and worsened mental health
The results of a 2021 international survey1 of 129 female-to-male patients who underwent genital reconstruction surgery support anecdotal reports that complication rates following genital reconstruction are higher than are commonly reported in the surgical literature.
Complication rates, including urethral compromise, and worsened mental health outcomes remain high for gender affirming penile reconstruction. In total, the 129 patients reported 281 complications requiring 142 revisions.
Another paper2 found a 70% complication rate in one type of female-to-male genital reconstruction surgery.
Even with the “radial forearm free flap” method of creating a synthetic penis — “considered by many as the gold standard for phalloplasty”3 — there are high rates of complications, with up to 64% urethroplasty related complications4.
- Robinson, I.S., Blasdel, G., Cohen, O., Zhao, L.C. & Bluebond-Langner, R. (2021). Surgical Outcomes Following Gender Affirming Penile Reconstruction: Patient-Reported Outcomes From a Multi-Center, International Survey of 129 Transmasculine Patients. J Sex Med 18 (4): 800-811. [Link] ↩︎
- Bettocchi, C., Ralph, D.J. & Pryor, J.P. (2005). Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int. 95:120–4. [Link] ↩︎
- Rashid, M. & Tamimy, M. S. (2013). Phalloplasty: The dream and the reality. Indian J Plast Surg 46 (2): 283-293. [Link] ↩︎
- Fang, R.H., Lin, J.T. & Ma S. (1994). Phalloplasty for female transsexuals with sensate free forearm flap. Microsurgery 15: 349–52. [Link] ↩︎
-
The profile of people seeking transition has shifted drastically, from overwhelmingly middle-aged males to predominantly adolescent females
A 2017 paper1 notes that “in adolescents, there has been a recent inversion in the sex ratio from one favouring birth-assigned males to one favouring birth-assigned females.” By contrast, over 90% of transsexual adults in the 1960s were male2.
In fact, there was hardly any scientific literature before 2012 on girls ages 11 to 21 ever having developed gender dysphoria at all. Yet of the young people described in Lisa Littman’s 2018 seminal paper on young people3, 82.8% were female.
The data for the UK’s Gender Identity Development Service4 show that 138 children were referred in 2011, and most of those children were boys. By 2021, however, a complete sex ratio reversal had occurred, and the clinic saw 2383 children that year, with almost 70% being female.
A 2017 article by Lisa Marchiano5 collated data from different clinics around the world and found international evidence for this shift in distribution.
- Zucker, K. J. (2017). Epidemiology of gender dysphoria and transgender identity. Sexual Health 14 (5): 404-411. [Link] ↩︎
- Barrett, J. (2015). Written evidence submitted by British Association of Gender Identity Specialists to the Transgender Equality Inquiry. data.parliament.uk [Link] ↩︎
- Littman, L. (2018). Rapid-onset gender dysphoria in adolescents and young adults: A study of parental reports. PLOS ONE, 13 (8). [Link] ↩︎
- Gender Identity Development Service (2021). Referrals to GIDS, financial years 2010-11 to 2020-21. [Link] ↩︎
- Marchiano, L. (2017). Outbreak: On Transgender Teens and Psychic Epidemics. Psychological Perspectives 60 (3): 345-366. [Link] ↩︎

