Category: Surgery
-
Rates of gender-affirming surgeries in the US tripled from 2016-2019.
A cohort study1 of data from the Nationwide Ambulatory Surgery Sample and the National Inpatient Sample showed that 48019 patients in the US received some kind of “gender-affirming” surgery between 2016 and 2020. Numbers peaked at 13011 in 2019 then fell slightly to 12818 in 2020. The study’s authors attribute this decline to the impact of the COVID-19 pandemic though, meaning the historical peak may not have been reached by then. 7.7% of all patients (3678 of the total) were aged 12-18 at the time of their surgery. 405 of these surgeries on minors (2.4% of the whole study) were genital surgeries. More than half (52.3%, or 25099 patients) were aged 19-30.
- Wright JD, Chen L, Suzuki Y, Matsuo K, Hershman DL. National Estimates of Gender-Affirming Surgery in the US. JAMA Network Open. 2023;6(8):e2330348. doi:10.1001/jamanetworkopen.2023.30348 ↩︎
-
Time until treatment regret emerges may be eight years or more.
An analysis1 showed that the median time to surgical regret may be as high as eight years. For cross-sex hormone treatment, the time to regret may be almost eleven years (130 months). However, the analysis points out that the lack of thorough follow up in much of the research in this field, and the lack of detailed research into the detransitioner/desister population, mean that accurate figures are very hard to discern.

- Cohn, J. The Detransition Rate Is Unknown. Archives of Sexual Behaviour 52, 1937–1952 (2023). https://doi.org/10.1007/s10508-023-02623-5 ↩︎
-
Quality Of Life scores start to decline around one year after “gender-affirming” surgery. After five years, these scores are below pre-surgery levels.
A systematic review and meta-analysis1 of studies on the Quality Of Life (QoL) of transgender patients showed that in every domain, these patients tended to have poor QoL compared to the general population. Some patients showed an increase in QoL in some domains, but this peaked after about a year. After five years, these scores were below pre-transition levels.
- Nobili, A., Glazebrook, C. & Arcelus, J. Quality of life of treatment-seeking transgender adults: A systematic review and meta-analysis. Rev Endocr Metab Disord 19, 199–220 (2018). https://doi.org/10.1007/s11154-018-9459-y ↩︎
-
36% of patients at Amsterdam gender clinic were lost to follow up.
In a study of all patients at a clinic treating 95% of all trans-identified people in the Netherlands1, 36% of all patients were lost to follow up. This may make reported rates of regret or detransition highly unreliable2. Rates of “regret” in the study itself may be compromised by a definition of “true regret” marked by beginning hormone therapy reflecting the patient’s sex (e.g. testosterone therapy for detransitioning “trans women” or estrogen therapy for detransitioning “trans men.”) The study also notes that some of those experiencing “true regret” had thought that transition would be a “solution” for their homosexuality. Regret was expressed between 46 and 271 months after beginning cross-sex hormone treatment. This may suggest there is a long tail of such regret still to come, even from those who began treatment more than twenty years ago.

- Wiepjes CM, Nota NM, de Blok CJM, Klaver M, de Vries ALC, Wensing-Kruger SA, de Jongh RT, Bouman MB, Steensma TD, Cohen-Kettenis P, Gooren LJG, Kreukels BPC, den Heijer M. The Amsterdam Cohort of Gender Dysphoria Study (1972-2015): Trends in Prevalence, Treatment, and Regrets. J Sex Med. 2018 Apr;15(4):582-590. doi: 10.1016/j.jsxm.2018.01.016. Epub 2018 Feb 17. PMID: 29463477 ↩︎
- https://catalogofbias.org/biases/attrition-bias/ ↩︎
-
Around 25–50% of transmen and 5–10% of transwomen have had genital surgery.
Based on a 2019 review, genital surgery1 as part of medical transition is generally less common than chest surgery, with reported rates of 25–50% for transmen (natal females) and 5–10% for transwomen (natal males). These estimates come from a range of surveys and clinical reports.
- Nolan, I. T., Kuhner, C. J., & Dy, G. W. (2019). Demographic and temporal trends in transgender identities and gender confirming surgery. Translational andrology and urology, 8(3), 184. [Link] ↩︎
-
“Gender-affirming” surgery is associated with increased risk of depression, anxiety, suicidal ideation, and substance use disorders.
A 2025 U.S. national database study1 examined over 107,000 adults diagnosed with gender dysphoria to compare those who did and did not undergo “gender-affirming” surgery. Using matched cohorts controlling for age, race, and ethnicity, the study found significantly higher risks of depression, anxiety, suicidal ideation, and substance use disorders within two years after surgery.
For males who had surgery, depression was 25.4% vs. 11.5% without surgery (RR 2.20) and anxiety 12.8% vs. 2.6% (RR 4.88). Females also showed increased rates: depression 22.9% vs. 14.6% (RR 1.56) and anxiety 10.5% vs. 7.1% (RR 1.48). Those undergoing feminizing procedures had particularly elevated risk for depression (RR 1.78) and substance use disorders (RR 1.28).
- Lewis, J. E., Patterson, A. R., Effirim, M. A., Patel, M. M., Lim, S. E., Cuello, V. A., … & Lee, W. C. (2025). Examining gender-specific mental health risks after gender-affirming surgery: a national database study. The Journal of Sexual Medicine, 22(4), 645-651. [Link] ↩︎
-
Genital surgery is associated with high rates of pelvic floor and sexual dysfunction.
A 2025 systematic review and meta-analysis1 examined 25 studies on pelvic floor outcomes after genital “gender-affirming” surgery. The findings show a high prevalence of complications among both male and female patients:
Type of Dysfunction Males (vaginoplasty) Females (hysterectomy & phalloplasty) Pelvic organ prolapse 1–7.5% 3.8% Urinary incontinence up to 15% up to 50% Urinary irritative symptoms up to 20% up to 37% Sexual dysfunction 25–75% 54% - Dominoni, M., Scatigno, A. L., Pasquali, M. F., Bergante, C., Gariboldi, F., & Gardella, B. (2025). Pelvic floor and sexual dysfunctions after genital gender-affirming surgery: a systematic review and meta-analysis. The Journal of Sexual Medicine, 22(1), 184-195. [Link] ↩︎
-
People who have undergone cross-sex surgery are over 19 times more likely to die by suicide than the general population
Dhejne et al. (2011)1 conducted the longest follow-up study to date on the outcomes of “sex reassignment surgery”, covering a period of 30 years (1973-2003) and involving 324 individuals in Sweden. The study compared these individuals to matched controls based on birth year and sex, revealing that those who had undergone surgery exhibited a significantly increased suicide risk, with rates nearly 19.1 times higher than their matched controls.
- Dhejne, C., Lichtenstein, P., Boman, M., Johansson, A. L., Långström, N., & Landén, M. (2011). Long-term follow-up of transsexual persons undergoing sex reassignment surgery: cohort study in Sweden. PloS one, 6(2), e16885. [Link] ↩︎
-
People who have undergone cross-sex surgery exhibit a significantly higher suicide risk
Dhejne et al. (2011)1 conducted the longest follow-up study to date on the outcomes of “sex reassignment surgery”, covering a period of 30 years (1973-2003) and involving 324 individuals in Sweden. The study compared these individuals to matched controls based on birth year and sex, revealing that those who had undergone surgery exhibited a significantly increased suicide risk, with rates nearly 19.1 times higher than their matched controls.
In the US, a 2024 study by Straub et al.2 analyzed the psychiatric risks of those who’ve undergone “gender-affirmation surgery” using a large patient dataset. This study compared individuals who had undergone the surgery to two control groups: one consisting of adults who had emergency department visits without any surgery and another comprising individuals who underwent either a tubal ligation or vasectomy. The findings indicated that those who had “gender-affirmation surgery” faced a 12.12-fold increased risk of attempting suicide compared to the emergency visit control group, and a 4.71-fold higher risk compared to the tubal ligation/vasectomy control group.
- Dhejne, C., Lichtenstein, P., Boman, M., Johansson, A. L., Långström, N., & Landén, M. (2011). Long-term follow-up of transsexual persons undergoing sex reassignment surgery: cohort study in Sweden. PloS one, 6(2), e16885. [Link] ↩︎
- Straub, J. J., Paul, K. K., Bothwell, L. G., Deshazo, S. J., Golovko, G., Miller, M. S., & Jehle, D. V. (2024). Risk of suicide and self-harm following gender-affirmation surgery. Cureus, 16(4). [Link] ↩︎
-
In one survey of WPATH-affiliated surgeons, over half reported performing vaginoplasty on minors
A 2017 study by Milrod and Karasic1 surveyed 20 WPATH-affiliated surgeons in the United States about their experiences and attitudes toward vaginoplasty in minors. Of these surgeons, 11 (55%) reported having performed the procedure on minors, with patient ages ranging from 15 to “a day before 18”.
- Milrod, C., & Karasic, D. H. (2017). Age is just a number: WPATH-affiliated surgeons’ experiences and attitudes toward vaginoplasty in transgender females under 18 years of age in the United States. The Journal of Sexual Medicine, 14(4), 624-634. [Link] ↩︎
-
Intestinal vaginoplasty in patients with stunted penile growth from puberty blockers can lead to bowel inflammation, excessive discharge, persistent foul odors, and fecal leakage
A 2017 survey by Milrod and Karasic1 found WPATH-affiliated surgeons in the United States considered sigmoid- or ileum-derived vaginoplasty (using sections of large or small intestine) an option for patients who had used puberty blockers. These patients, who had sometimes used blockers for up to 3 years, had severely underdeveloped genitals, described as “11-year-old genitalia” or a “micropenis,” which complicated standard surgical techniques. However, this intestinal approach was associated with serious complications, including diversion colitis (inflammation of the repurposed bowel tissue), excessive secretion, persistent foul odors, and potential leakage of stool into the peritoneum (the membrane lining the abdominal cavity).
- Milrod, C., & Karasic, D. H. (2017). Age is just a number: WPATH-affiliated surgeons’ experiences and attitudes toward vaginoplasty in transgender females under 18 years of age in the United States. The Journal of Sexual Medicine, 14(4), 624-634. [Link] ↩︎
-
Genital masculinizing surgeries rose by 424% and feminizing surgeries by 343% in Germany between 2006 and 2022
A 2024 German national study1 analyzing hospital records found that genital “gender-affirming” surgeries increased nearly 5-fold between 2006 and 2022. Masculinizing surgeries showed the most dramatic increase at 424%, with their highest annual rise occurring between 2018-2019, while feminizing surgeries increased by 343%, with their steepest rise between 2015-2016. The study found a dramatic shift toward younger patients, with over 70% of masculinizing and about half of feminizing surgeries performed on people aged 20-34 in 2022, compared to about a quarter for both types in 2006. These procedures became increasingly concentrated in specialized centers, with half of hospitals performing over 50 masculinizing surgeries annually by 2022, up from 15% in 2006.
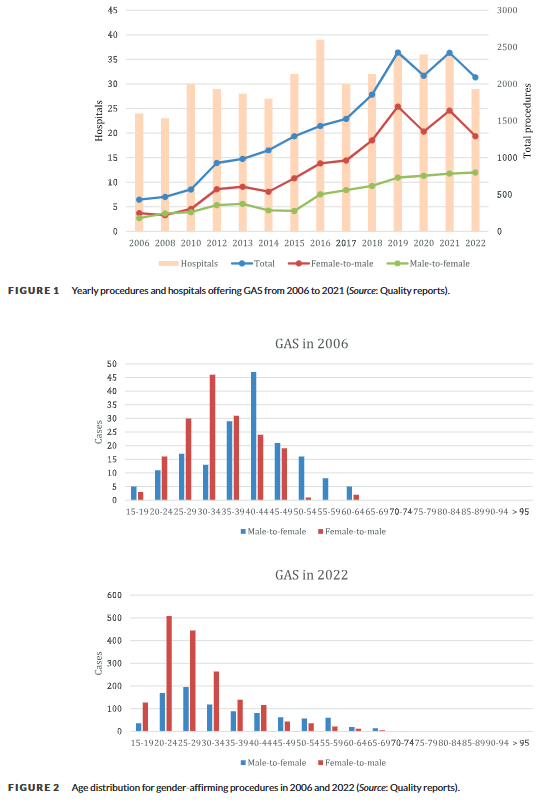
- Aksoy, C., Wellenbrock, S., Reimold, P., Karschuck, P., Ozturk, M., Hirsch, T., … & Flegar, L. (2024). Genital gender‐affirming surgery trends in Germany: Total population data with 19,600 cases from 2006 to 2022. Andrology. [Link] ↩︎
-
There is evidence that up to a quarter of transgender genital surgeries result in incontinence
A systematic literature review1 found that 21% of male-to-female patients and 25% of female-to-male patients suffered from incontinence as a result of transgender genital surgery.
One recent study2 estimates the number of post-operative transsexuals suffering stress incontinence to be 23%. This study was not a literature review, and almost all of the participants were male-to-female.
- Nassiri, N., Maas, M., Basin, M., Cacciamani, G.E. & Doumanian, L.R. (2020). Urethral complications after gender reassignment surgery: a systematic review. Int J Impot Res. [Link] ↩︎
- Kuhn, A., Santi, A. & Birkhäuser, M. (2011). Vaginal prolapse, pelvic floor function, and related symptoms 16 years after sex reassignment surgery in transsexuals. Fertil Steril. 95: 2379-82. [Link] ↩︎
-
Around 1 in 5 vaginoplasty surgeries lead to corrective surgery
A systematic review1 of neo-vagina surgeries found a re-operation rate of 21.7% for non-esthetic reasons.
A Brazilian paper2 found a somewhat lower, but similar, reoperation rate of 16.8%.
- Dreher, P.C., Edwards, D., Hager, S., Dennis, M., Belkoff, A., Mora, J., Tarry, S. & Rumer, K.L. (2018). Complications of the neovagina in male-to-female transgender surgery: A systematic review and meta-analysis with discussion of management. Clin Anat. 31 (2):191-199. [Link] ↩︎
- Moisés da Silva, G.V., Lobato, M.I.R., Silva, D.C., Schwarz, K., Fontanari, A.M.V., Costa, A.B., Tavares, P.M., Gorgen, A.R.H., Cabral, R.D. & Rosito, T.E. (2021). Male-to-Female Gender-Affirming Surgery: 20-Year Review of Technique and Surgical Results. Frontiers in Surgery 8. [Link] ↩︎
-
Vaginoplasty can result in fistula, stenosis, necrosis, prolapse and even death
Male-to-female genital surgery (vaginoplasty) is associated with significant long-term complications: there is a 2% risk of fistula, 14% risk of stenosis (abnormal narrowing), 1% risk of necrosis (tissue death) and 4% risk of prolapse1.
One systematic review2 found an overall complication rate of 32.5%.
A Dutch study3 of 55 (out of an original 70) adolescents treated with puberty blockers, cross sex hormones, and genital surgery, showed that among 22 male-to-female patients who underwent vaginoplasty, one adolescent died as a result of necrotizing fasciitis after the surgery.
- Manrique, O., Adabi, K., Martinez-Jorge, J., Ciudad, P., Nicoli, F. and Kiranantawat, K. (2018). Complications and Patient-Reported Outcomes in Male-to-Female Vaginoplasty—Where We Are Today. Annals of Plastic Surgery 80 (6): 684-691. [Link] ↩︎
- Dreher, P.C., Edwards, D., Hager, S., Dennis, M., Belkoff, A., Mora, J., Tarry, S. & Rumer, K.L. (2018). Complications of the neovagina in male-to-female transgender surgery: A systematic review and meta-analysis with discussion of management. Clin Anat. 31 (2):191-199. [Link] ↩︎
- de Vries, A., McGuire, T., Steensma, E., Wagenaar, T., Doreleijers, P. & Cohen-Kettenis, P. (2014). Young adult psychological outcome after puberty suppression and gender reassignment. [Link] ↩︎
-
Genital surgeries tend to reduce the capacity for orgasm in males, and may do so in females
One study showed that around 30% of male-to-female genital surgeries result in the inability to orgasm1.
Figures on female-to-male transitioners are less clear. However, a clinical follow-up study2 of 38 transmen – 29 of whom had received phalloplasty, and 9 metoidioplasty – found that reported loss of orgasmic capacity was more marginally common than reported gain of orgasmic capacity.
The negative intrapsychic and interpersonal consequences of anorgasmia (the inability to climax) is well-documented, and applies equally to transgender individuals3.
- Manrique, O., Adabi, K., Martinez-Jorge, J., Ciudad, P., Nicoli, F. and Kiranantawat, K. (2018). Complications and Patient-Reported Outcomes in Male-to-Female Vaginoplasty—Where We Are Today. Annals of Plastic Surgery 80 (6): 684-691. [Link] ↩︎
- van de Grift, T., Pigot, G., Kreukels, B., Bouman, M., & Mullender, M. (2019). Transmen’s Experienced Sexuality and Genital Gender-Affirming Surgery: Findings From a Clinical Follow-Up Study. Journal Of Sex & Marital Therapy 45 (3): 201-205. [Link] ↩︎
- Levine, S. (2018). Informed Consent for Transgendered Patients. Journal Of Sex & Marital Therapy, 45(3), 218-229. [Link] ↩︎
-
Medical transition puts both males and females at risk of infertility
A wide-ranging study1 found that gender-related drug regimens place patients at risk of infertility:
Suppression of puberty with gonadotropin-releasing hormone agonist analogs (GnRHa) in the pediatric transgender patient can pause the maturation of germ cells, and thus, affect fertility potential. Testosterone therapy in transgender men can suppress ovulation and alter ovarian histology, while estrogen therapy in transgender women can lead to impaired spermatogenesis and testicular atrophy. The effect of hormone therapy on fertility is potentially reversible, but the extent is unclear.
On surgeries, the study noted that cross-sex surgery that includes hysterectomy and oophorectomy in transmen or orchiectomy in transwomen results in permanent sterility.
- Cheng, P.J., Pastuszak, A.W., Myers, J.B., Goodwin, I.A. & Hotaling, J.M. (2019). Fertility concerns of the transgender patient. Transl Androl Urol. 8 (3): 209-218. [Link] ↩︎
-
Female-to-male genital reconstruction surgery has a high negative outcome rate, including urethral compromise and worsened mental health
The results of a 2021 international survey1 of 129 female-to-male patients who underwent genital reconstruction surgery support anecdotal reports that complication rates following genital reconstruction are higher than are commonly reported in the surgical literature.
Complication rates, including urethral compromise, and worsened mental health outcomes remain high for gender affirming penile reconstruction. In total, the 129 patients reported 281 complications requiring 142 revisions.
Another paper2 found a 70% complication rate in one type of female-to-male genital reconstruction surgery.
Even with the “radial forearm free flap” method of creating a synthetic penis — “considered by many as the gold standard for phalloplasty”3 — there are high rates of complications, with up to 64% urethroplasty related complications4.
- Robinson, I.S., Blasdel, G., Cohen, O., Zhao, L.C. & Bluebond-Langner, R. (2021). Surgical Outcomes Following Gender Affirming Penile Reconstruction: Patient-Reported Outcomes From a Multi-Center, International Survey of 129 Transmasculine Patients. J Sex Med 18 (4): 800-811. [Link] ↩︎
- Bettocchi, C., Ralph, D.J. & Pryor, J.P. (2005). Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int. 95:120–4. [Link] ↩︎
- Rashid, M. & Tamimy, M. S. (2013). Phalloplasty: The dream and the reality. Indian J Plast Surg 46 (2): 283-293. [Link] ↩︎
- Fang, R.H., Lin, J.T. & Ma S. (1994). Phalloplasty for female transsexuals with sensate free forearm flap. Microsurgery 15: 349–52. [Link] ↩︎

