Category: Medical transition • Page 2
-
There is no high-quality evidence supporting the use of puberty blockers for gender distress
A 2024 systematic review by Taylor et al. at the University of York1 was commissioned by the Cass Review to rigorously assess the safety and effectiveness of puberty suppression in adolescents with gender dysphoria. Analyzing studies up to April 2022, the review included 11 cohort, 8 cross-sectional, and 31 pre-post studies, but only one cross-sectional study met high-quality standards. The meta-analysis of moderate to high-quality studies showed limited and inconsistent evidence of benefits in areas like gender dysphoria, mental health, and body satisfaction.
This finding aligns with the previous 2020 review by the British National Institute for Clinical Excellence (NICE) on puberty blockers2, which described the supporting evidence as “very low” quality. The review noted minimal changes in key outcomes like gender dysphoria, mental health, and quality of life due to small, uncontrolled observational studies. Furthermore, a 2024 review from Germany by Zepf et al.3, adhering to NICE criteria, confirmed the absence of new studies on puberty blockers for gender dysphoria since the NICE review.
- Taylor, J., Mitchell, A., Hall, R., Heathcote, C., Langton, T., Fraser, L., & Hewitt, C. E. (2024). Interventions to suppress puberty in adolescents experiencing gender dysphoria or incongruence: a systematic review. Archives of disease in childhood, archdischild-2023-326669. [Link] ↩︎
- National Institute for Health and Care Excellence (2021). Evidence review: Gonadotrophin releasing hormone analogues for children and adolescents with gender dysphoria. National Institute for Health and Care Excellence (NICE); NHS England; NHS Improvement. [Link] ↩︎
- Zepf, F. D., König, L., Kaiser, A., Ligges, C., Ligges, M., Roessner, V., … & Holtmann, M. (2024). Beyond NICE: Aktualisierte systematische Übersicht zur Evidenzlage der Pubertätsblockade und Hormongabe bei Minderjährigen mit Geschlechtsdysphorie. Zeitschrift für Kinder-und Jugendpsychiatrie und Psychotherapie. [Link] ↩︎
-
In one survey of WPATH-affiliated surgeons, over half reported performing vaginoplasty on minors
A 2017 study by Milrod and Karasic1 surveyed 20 WPATH-affiliated surgeons in the United States about their experiences and attitudes toward vaginoplasty in minors. Of these surgeons, 11 (55%) reported having performed the procedure on minors, with patient ages ranging from 15 to “a day before 18”.
- Milrod, C., & Karasic, D. H. (2017). Age is just a number: WPATH-affiliated surgeons’ experiences and attitudes toward vaginoplasty in transgender females under 18 years of age in the United States. The Journal of Sexual Medicine, 14(4), 624-634. [Link] ↩︎
-
Intestinal vaginoplasty in patients with stunted penile growth from puberty blockers can lead to bowel inflammation, excessive discharge, persistent foul odors, and fecal leakage
A 2017 survey by Milrod and Karasic1 found WPATH-affiliated surgeons in the United States considered sigmoid- or ileum-derived vaginoplasty (using sections of large or small intestine) an option for patients who had used puberty blockers. These patients, who had sometimes used blockers for up to 3 years, had severely underdeveloped genitals, described as “11-year-old genitalia” or a “micropenis,” which complicated standard surgical techniques. However, this intestinal approach was associated with serious complications, including diversion colitis (inflammation of the repurposed bowel tissue), excessive secretion, persistent foul odors, and potential leakage of stool into the peritoneum (the membrane lining the abdominal cavity).
- Milrod, C., & Karasic, D. H. (2017). Age is just a number: WPATH-affiliated surgeons’ experiences and attitudes toward vaginoplasty in transgender females under 18 years of age in the United States. The Journal of Sexual Medicine, 14(4), 624-634. [Link] ↩︎
-
There is a significant burden of chronic pain in trans-identified individuals, with an increased risk among those receiving cross-sex hormones
A 2024 large US clinical database study1 of 98,352 trans-identified individuals (56,470 females and 41,882 males) found significantly higher rates of chronic pain compared to the general population. Of particular concern, those receiving cross-sex hormones showed even higher risks – females on testosterone had a 20% increased hazard of chronic pain diagnosis compared to those not taking testosterone, while males on estrogen showed a 19.4% increased risk.
- Tabernacki, T., Gilbert, D., Rhodes, S., Scarberry, K., Pope, R., McNamara, M., … & Mishra, K. (2024). The burden of chronic pain in transgender and gender diverse populations: Evidence from a large US clinical database. European Journal of Pain. [Link] ↩︎
-
Genital masculinizing surgeries rose by 424% and feminizing surgeries by 343% in Germany between 2006 and 2022
A 2024 German national study1 analyzing hospital records found that genital “gender-affirming” surgeries increased nearly 5-fold between 2006 and 2022. Masculinizing surgeries showed the most dramatic increase at 424%, with their highest annual rise occurring between 2018-2019, while feminizing surgeries increased by 343%, with their steepest rise between 2015-2016. The study found a dramatic shift toward younger patients, with over 70% of masculinizing and about half of feminizing surgeries performed on people aged 20-34 in 2022, compared to about a quarter for both types in 2006. These procedures became increasingly concentrated in specialized centers, with half of hospitals performing over 50 masculinizing surgeries annually by 2022, up from 15% in 2006.
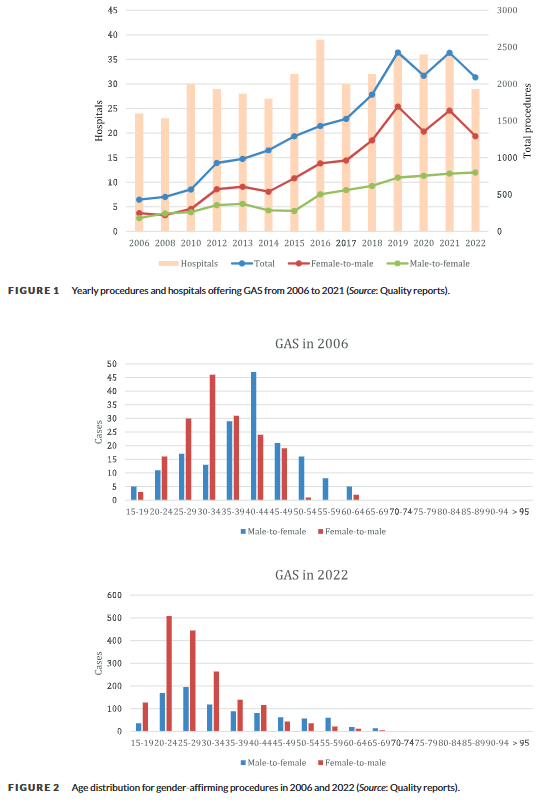
- Aksoy, C., Wellenbrock, S., Reimold, P., Karschuck, P., Ozturk, M., Hirsch, T., … & Flegar, L. (2024). Genital gender‐affirming surgery trends in Germany: Total population data with 19,600 cases from 2006 to 2022. Andrology. [Link] ↩︎
-
Suppressing sex hormones in males, using treatments like those prescribed as puberty blockers, is linked to an increased risk of dementia
A 2025 systematic review and meta-analysis1 found that men receiving androgen deprivation therapy (ADT) for prostate cancer had an increased risk of dementia, with a 26% higher likelihood for all types of dementia and a 9% higher risk specifically for Alzheimer’s disease, compared to men not receiving this treatment. ADT reduces the effects of male sex hormones (androgens) such as testosterone and dihydrotestosterone (DHT). This is achieved using medications, including GnRH agonists (which initially stimulate and then suppress hormone production via the pituitary gland), GnRH antagonists (which directly block hormone receptor activity), or through other pharmaceutical and surgical approaches. Notably, some of the same medications used for ADT—GnRH agonists, GnRH antagonists, and certain antiandrogens—are also employed as “puberty blockers” to delay puberty in children and adolescents.
- Ma, L., Tan, E. C., Goudey, B., Jin, L., & Pan, Y. (2025). Unraveling the bidirectional link between cancer and dementia and the impact of cancer therapies on dementia risk: A systematic review and meta‐analysis. Alzheimer’s & Dementia, e14540. [Link] ↩︎
-
Long term testosterone use potentially compromises fertility and negatively affects ovarian follicle health
One study in 2023 found that long-term testosterone exposure, as seen in transgender men undergoing gender-affirming therapy, could potentially compromise fertility by negatively affecting ovarian follicle growth, health, and DNA integrity.
In 2023, a study by Bailie et al1. explored the effects of long-term testosterone exposure on ovarian follicles in transgender men receiving gender-affirming endocrine therapy. The research indicated that testosterone was linked with decreased follicle growth activation, poor follicle health, and increased DNA damage, suggesting possible impacts on fertility. Further, these negative effects were intensified following six days of in vitro culture. These findings may have crucial implications for reproductive health and fertility considerations among transgender men receiving testosterone as part of their gender-affirming therapy.
- Bailie, E., Maidarti, M., Hawthorn, R., Jack, S., Watson, N., Telfer, E. E., & Anderson, R. A. (2023). The ovaries of transgender men indicate effects of high dose testosterone on the primordial and early growing follicle pool. Reproduction and Fertility, 4(2). [Link] ↩︎
-
One year of cross sex hormone therapy causes robust increases in muscle mass and strength in transmen (females) but modest changes in transwomen (males)
Thigh muscle volume increased 15% in transmen, which was paralleled by increased quadriceps cross-sectional area (CSA) (15%) and radiological density 6%. In transwomen, the corresponding parameters decreased by –5% (muscle volume) and –4% (CSA), while density remained unaltered. The transmen increased strength over the assessment period, while the transwomen generally maintained their strength levels1:

- Wiik, A., Lundberg, T. R., Rullman, E., Andersson, D. P., Holmberg, et al. (2019). Muscle strength, size, and composition following 12 months of gender-affirming treatment in transgender individuals. The Journal of Clinical Endocrinology & Metabolism, 105(3). [Link] ↩︎
-
Strength advantage over females is retained by male-to-female transitioners (transwomen)
A systematic review of 24 studies concluded that while male-female transitioners (transwomen) do experience some decrease in muscle mass; values for strength and muscle area in transwomen remain above those of biological women, even after 36 months of hormone therapy.
Figure one1:

The above graph show’s the performance difference between transwomen and biological women in various sports. A systematic review of 24 studies concluded that while male-female transitioners (trans women) do experience a decrease in muscle mass; values for strength and muscle area in transwomen remain above those of biological women, even after 36 months of hormone therapy2.
- Hilton, E. N. & Lundberg, T.R. (2021). Transgender Women in the Female Category of Sport: Perspectives on Testosterone Suppression and Performance Advantage. Sports Med 51: 199–214. [Link] ↩︎
- Harper J, O’Donnell E, Sorouri Khorashad B, et al . (2021). How does hormone transition in transgender women change body composition, muscle strength and haemoglobin? Systematic review with a focus on the implications for sport participation. British Journal of Sports Medicine ;55:865-872. [Link] ↩︎
-
In one study of detransitioners, around half believed that they received inadequate care
The majority (55.0%) of detransitioners in a 100-participant study1 felt that they did not receive an adequate evaluation from a doctor or mental health professional before starting transition.
A second study2 of detransitioners and desisters – most of whom were detransitioners who had undergone medical transition – arrived at a similar, although slightly lower, figure, with 45% of detransitioners not feeling properly informed about the health implications of the accessed treatments and interventions before undergoing them.
- Littman, L. (2021). Individuals Treated for Gender Dysphoria with Medical and/or Surgical Transition Who Subsequently Detransitioned: A Survey of 100 Detransitioners. Arch Sex Behav. [Link] ↩︎
- Vandenbussche, E. (2021). Detransition-Related Needs and Support: A Cross-Sectional Online Survey. Journal of Homosexuality. [Link] ↩︎
-
In one study of detransitioners, around half were worried about the medical complications of transitioning
A study1 of 100 detransitioners showed that 49% had concerns about potential medical complications from transitioning.
A second study2 of detransitioners and desisters – most of whom were detransitioners who had undergone medical transition – arrived at a higher figure, with 62% citing health concerns as a motivating factor for detransition.
- Littman, L. (2021). Individuals Treated for Gender Dysphoria with Medical and/or Surgical Transition Who Subsequently Detransitioned: A Survey of 100 Detransitioners. Arch Sex Behav. [Link] ↩︎
- Vandenbussche, E. (2021). Detransition-Related Needs and Support: A Cross-Sectional Online Survey. Journal of Homosexuality. [Link] ↩︎
-
Transmen are four or five times more likely than females in general to suffer a heart attack
A 2019 study1 found that post-operative female-to-male transgender people were 4.9 times as likely to suffer a myocardial infarction (heart attack) than women in general.
Another study2 also found a somewhat smaller yet still large discrepancy, concluding that transmen were 3.69 more likely to suffer a heart attack than women in general.
- Alzahrani, T. Nguyen, T., Ryan, A., Dwairy, A. McCaffrey, J., Yunus, R., Forgione, J., Krepp, J., Nagy, C., Mazhari, R. & Reiner, J. (2019). Cardiovascular Disease Risk Factors and Myocardial Infarction in the Transgender Population. Circulation: Cardiovascular Quality and Outcomes 12 (4). [Link] ↩︎
- Nota, N.M., Wiepjes, C.M., de Blok, C.J.M., Gooren, L.J.G., Kreukels, B.P.D. & den Heijer, M. (2019). Occurrence of Acute Cardiovascular Events in Transgender Individuals Receiving Hormone Therapy: Results From a Large Cohort Study. Circulation 139: 1461-1462. [Link] ↩︎
-
There is evidence that it is harder to sustain meaningful sexual relationships after medical transition
A study1 on informed consent found that male-to-female transitioners who are attracted to men may discover that men who are sexually interested in them are specifically interested in their trans status, and have no interest in serious long-term relationships.
The same study noted that male-to-female transitioners who are attracted to women may find that lesbians are unwilling to engage in a sexual relationship with a male.
Because most female-to-male transitioners do not undergo phalloplasty, their ability to attract desirable sexual partners, and sustain relationships with them, could be compromised.
Only a single case2 of a female-to-male transitioner treated with puberty blockers followed by cross-sex hormones and surgeries has feen followed long-term.
The individual, who was in his thirties during the follow up, reported an inability to have a satisfying sexual life due to “shame about his genital appearance and his feelings of inadequacy in sexual matters”. The researchers concluded, that despite the gender reassignment, “in the area of intimate relationships, it may remain difficult to find a suitable partner”.
- Levine, S. (2018). Informed Consent for Transgendered Patients. Journal Of Sex & Marital Therapy, 45(3), 218-229. [Link] ↩︎
- Cohen-Kettenis, P., Schagen, S., Steensma, T., de Vries, A., & Delemarre-van de Waal, H. (2011). Puberty Suppression in a Gender-Dysphoric Adolescent: A 22-Year Follow-Up. Archives Of Sexual Behavior 40 (4): 843-847. [Link] ↩︎
-
Medical transition reduces dating pool size and likelihood of marriage
Individuals undergoing biomedical interventions to address their gender dysphoria are at risk for having a greatly diminished pool of individuals who are willing to sustain an intimate physical and loving relationship1.
This is evidenced in the much lower marriage rates of transgender adults2.
- Levine, S. (2018). Informed Consent for Transgendered Patients. Journal Of Sex & Marital Therapy, 45(3), 218-229. [Link] ↩︎
- Yarbrough, E. (2018). Transgender mental health. Washington, DC: American Psychiatric Association Publishing. [Link] ↩︎
-
There is evidence that up to a quarter of transgender genital surgeries result in incontinence
A systematic literature review1 found that 21% of male-to-female patients and 25% of female-to-male patients suffered from incontinence as a result of transgender genital surgery.
One recent study2 estimates the number of post-operative transsexuals suffering stress incontinence to be 23%. This study was not a literature review, and almost all of the participants were male-to-female.
- Nassiri, N., Maas, M., Basin, M., Cacciamani, G.E. & Doumanian, L.R. (2020). Urethral complications after gender reassignment surgery: a systematic review. Int J Impot Res. [Link] ↩︎
- Kuhn, A., Santi, A. & Birkhäuser, M. (2011). Vaginal prolapse, pelvic floor function, and related symptoms 16 years after sex reassignment surgery in transsexuals. Fertil Steril. 95: 2379-82. [Link] ↩︎
-
Around 1 in 5 vaginoplasty surgeries lead to corrective surgery
A systematic review1 of neo-vagina surgeries found a re-operation rate of 21.7% for non-esthetic reasons.
A Brazilian paper2 found a somewhat lower, but similar, reoperation rate of 16.8%.
- Dreher, P.C., Edwards, D., Hager, S., Dennis, M., Belkoff, A., Mora, J., Tarry, S. & Rumer, K.L. (2018). Complications of the neovagina in male-to-female transgender surgery: A systematic review and meta-analysis with discussion of management. Clin Anat. 31 (2):191-199. [Link] ↩︎
- Moisés da Silva, G.V., Lobato, M.I.R., Silva, D.C., Schwarz, K., Fontanari, A.M.V., Costa, A.B., Tavares, P.M., Gorgen, A.R.H., Cabral, R.D. & Rosito, T.E. (2021). Male-to-Female Gender-Affirming Surgery: 20-Year Review of Technique and Surgical Results. Frontiers in Surgery 8. [Link] ↩︎
-
Vaginoplasty can result in fistula, stenosis, necrosis, prolapse and even death
Male-to-female genital surgery (vaginoplasty) is associated with significant long-term complications: there is a 2% risk of fistula, 14% risk of stenosis (abnormal narrowing), 1% risk of necrosis (tissue death) and 4% risk of prolapse1.
One systematic review2 found an overall complication rate of 32.5%.
A Dutch study3 of 55 (out of an original 70) adolescents treated with puberty blockers, cross sex hormones, and genital surgery, showed that among 22 male-to-female patients who underwent vaginoplasty, one adolescent died as a result of necrotizing fasciitis after the surgery.
- Manrique, O., Adabi, K., Martinez-Jorge, J., Ciudad, P., Nicoli, F. and Kiranantawat, K. (2018). Complications and Patient-Reported Outcomes in Male-to-Female Vaginoplasty—Where We Are Today. Annals of Plastic Surgery 80 (6): 684-691. [Link] ↩︎
- Dreher, P.C., Edwards, D., Hager, S., Dennis, M., Belkoff, A., Mora, J., Tarry, S. & Rumer, K.L. (2018). Complications of the neovagina in male-to-female transgender surgery: A systematic review and meta-analysis with discussion of management. Clin Anat. 31 (2):191-199. [Link] ↩︎
- de Vries, A., McGuire, T., Steensma, E., Wagenaar, T., Doreleijers, P. & Cohen-Kettenis, P. (2014). Young adult psychological outcome after puberty suppression and gender reassignment. [Link] ↩︎
-
Feminizing hormones reduce sexual function in males
Feminizing hormonal treatments lead to a lessening drive, erectile dysfunction, and shrinking of testes and penis1, significantly compromising sexual function.
A Belgian doctoral thesis study2 found that 69.7% of transwomen reported a decrease in sexual desire — while the opposite effect is found in transmen.
- Levine, S. (2018). Informed Consent for Transgendered Patients. Journal Of Sex & Marital Therapy, 45(3), 218-229. [Link] ↩︎
- Elaut, E. (2014). Biopsychosocial factors in the sexual desire of contraception‐using couples and trans persons. Doctoral thesis, University of Ghent. [Link] ↩︎
-
Genital surgeries tend to reduce the capacity for orgasm in males, and may do so in females
One study showed that around 30% of male-to-female genital surgeries result in the inability to orgasm1.
Figures on female-to-male transitioners are less clear. However, a clinical follow-up study2 of 38 transmen – 29 of whom had received phalloplasty, and 9 metoidioplasty – found that reported loss of orgasmic capacity was more marginally common than reported gain of orgasmic capacity.
The negative intrapsychic and interpersonal consequences of anorgasmia (the inability to climax) is well-documented, and applies equally to transgender individuals3.
- Manrique, O., Adabi, K., Martinez-Jorge, J., Ciudad, P., Nicoli, F. and Kiranantawat, K. (2018). Complications and Patient-Reported Outcomes in Male-to-Female Vaginoplasty—Where We Are Today. Annals of Plastic Surgery 80 (6): 684-691. [Link] ↩︎
- van de Grift, T., Pigot, G., Kreukels, B., Bouman, M., & Mullender, M. (2019). Transmen’s Experienced Sexuality and Genital Gender-Affirming Surgery: Findings From a Clinical Follow-Up Study. Journal Of Sex & Marital Therapy 45 (3): 201-205. [Link] ↩︎
- Levine, S. (2018). Informed Consent for Transgendered Patients. Journal Of Sex & Marital Therapy, 45(3), 218-229. [Link] ↩︎
-
In one study, 11% of transmen who took testosterone developed a condition called erythrocytosis, which impacts red blood cells and slows the blood flow
A study1 of 776 transmen who took testosterone demonstrated that 11% of them developed erythrocytosis, a condition which slows the blood flow, and can lead to headaches, confusion, high blood pressure, nosebleeds, blurred vision, itching and fatigue.
- Madsen, M.C., van Dijk, D. Wiepjes, C.M., Conemans, E.B., Thijs, A. & den Heijer, M. (2021). Erythrocytosis in a Large Cohort of Trans Men Using Testosterone: A Long-Term Follow-Up Study on Prevalence, Determinants, and Exposure Years. The Journal of Clinical Endocrinology & Metabolism 106 (6): 1710–1717. [Link] ↩︎

